InBra electric
Introducing Medela's next generation breast pump InBra™ electric breast pumps,

Hands-free Electric
Hands-free breast pumps with in-bra collection cups and a rechargeable battery for easy multi-tasking. Available in single or double cups.

Classic Electric
Classic electric breast pumps with 2-Phase Expression mimic natural sucking, helping mums express more milk in less time. Explore now!
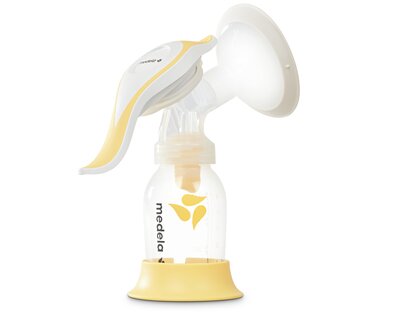
Manual
Manual breast pumps are ideal for mums who express occasionally and need a lightweight, portable solution for travel. Discover now!

Symphony - No 1 hospital pump and sets
Medela Symphony® is a reliable, multi-user breast pump for hospitals and home rental, ideal for long-term and frequent pumping.

Hands-free set

Traditional kit
The PersonalFit Flex™ breast pump kit has everything you need to go with your Medela Freestyle™ or Swing Maxi™ electric breast pump.

Shields
Check out our selection of breast shields designed to enhance your pumping experience and provide maximum comfort.

Membranes
Membranes are essential components in breast pump systems, including hands-free membranes for Medela Hands-free collection cups and replacement protective cap & membranes for the Medela Symphony®

Connectors
With our new PersonalFit Flex™ connector, you can pump in a more reclined and comfortable position.

Tubing
Replacement tubing tested and designed.

Power units
Authentic replacement power adapter for your Medela breast pumps.

Pumping garments
Explore Medela's Pumping Bras and Bustiers for effortless breastfeeding and pumping. Experience comfort and convenience. Learn more!

Maternity & nursing bras
Explore Medela's maternity bras and bralettes for nursing, designed for comfort and easy breastfeeding. Perfect for new and expectant mothers. Learn more!


InBra electric
Introducing Medela's next generation breast pump InBra™ electric breast pumps,

Hands-free Electric
Hands-free breast pumps with in-bra collection cups and a rechargeable battery for easy multi-tasking. Available in single or double cups.

Classic Electric
Classic electric breast pumps with 2-Phase Expression mimic natural sucking, helping mums express more milk in less time. Explore now!

Manual
Manual breast pumps are ideal for mums who express occasionally and need a lightweight, portable solution for travel. Discover now!

Symphony - No 1 hospital pump and sets
Medela Symphony® is a reliable, multi-user breast pump for hospitals and home rental, ideal for long-term and frequent pumping.

Hands-free set

Traditional kit
The PersonalFit Flex™ breast pump kit has everything you need to go with your Medela Freestyle™ or Swing Maxi™ electric breast pump.

Shields
Check out our selection of breast shields designed to enhance your pumping experience and provide maximum comfort.

Membranes
Membranes are essential components in breast pump systems, including hands-free membranes for Medela Hands-free collection cups and replacement protective cap & membranes for the Medela Symphony®

Connectors
With our new PersonalFit Flex™ connector, you can pump in a more reclined and comfortable position.

Tubing
Replacement tubing tested and designed.

Power units
Authentic replacement power adapter for your Medela breast pumps.

Pumping garments
Explore Medela's Pumping Bras and Bustiers for effortless breastfeeding and pumping. Experience comfort and convenience. Learn more!

Maternity & nursing bras
Explore Medela's maternity bras and bralettes for nursing, designed for comfort and easy breastfeeding. Perfect for new and expectant mothers. Learn more!

Magic InBra™
Medela Magic InBra: The gentle wearable breast pump for unmatched performance
Meet the next generation breast pump combining unmatched performance, comfort and discretion so mums never have to compromise again.

Symphony® breast pump
The Symphony breast pump by Medela is a double electric hospital-grade breast pump available for rental.